Cardiac myxoma originating from mitral valve leaflet
- Authors: Vishniakova M.V.1, Abramenko A.S.1, Vishniakova M.V.1, Shumakov D.V.1
-
Affiliations:
- Moscow Regional Research and Clinical Institute
- Issue: Vol 3, No 1 (2022)
- Pages: 64-70
- Section: Case reports
- Submitted: 07.02.2022
- Accepted: 07.04.2022
- Published: 24.04.2022
- URL: https://jdigitaldiagnostics.com/DD/article/view/100281
- DOI: https://doi.org/10.17816/DD100281
- ID: 100281
Cite item
Abstract
Primary heart tumors are an extremely rare disease, with a prevalence of 0.0017%–0.03% in the population according to various data.
Heart tumors are benign in most cases, and more than half of such formations are represented by cardiac myxomas. Myxoma is the most common primary cardiac tumor; however, its number is extremely small among the general population. Myxoma that affects the cardiac valves is a rare pathology. For the first time, such variance of changes was described in 1934. Most often, cardiac myxomas are localized at the atrial septum level near the oval fossa. One of the typical signs of myxoma is a narrow leg and an uneven surface, which causes the risk of embolism. Echocardiographic examination and magnetic resonance imaging are currently the methods of choice when suspecting the presence of volumetric heart formation. With such atypical tumor localization, conducting a mandatory differential diagnosis with heart valve vegetations and papillary fibroelastoma is necessary.
Herein, presented an elderly patient with complaints of shortness of breath, stabbing pains in the left half of the chest, and arrhythmias with a history of aspiration pneumonia and esophageal extirpation with stomach esophagogastroplasty. During the examination, the patient revealed a paroxysmal form of atrial fibrillation (outside of paroxysm), chronic heart failure, and arterial hypertension. The clinical data of the patient were not characteristic enough for the possibility of infectious endocarditis with valvular vegetations. The echocardiographic examination and multispiral computed tomography with bolus contrast enhancement on the atrial surface of the posterior flap of the mitral valve revealed an additional volume formation of 5–9 mm in size, rounded shape, with clear uneven contours, together with the valve flap into the left ventricular cavity into the atrial systole. The formation was optimally visualized using the Fiesta-CINE mode in modified two- and four-chamber projections. The formation was removed with suture plasty of the mitral valve in artificial blood circulation conditions. The histological examination of the formation revealed a morphological characteristic of myxoma. The postoperative period proceeded without complications.
Full Text
INTRODUCTION
Primary cardiac tumor is an extremely rare disease. According to different data, their prevalence in the population is 0.0017%–0.03% [1, 2]. Cardiac tumors are benign in most cases, of which more than half are represented by cardiac myxomas [3–7].
Myxomas are believed to originate from residual fragments of multipotent mesenchymal cells in the endocardium. Cardiac myxomas are most commonly located at the interatrial septum level near the oval fossa. One of the typical features of myxomas is a narrow pedicle and an irregular surface, which leads to the risk of embolism in this type of tumor.
CLINICAL CASE
Patient T, a 64-year-old female patient, was admitted with complaints of dyspnea, stabbing pain in the left side of the chest, and arrhythmia. Her medical history included aspiration pneumonia and esophageal extirpation with gastric esophagogastroplasty.
Physical, laboratory, and instrumental findings
The examination revealed a paroxysmal form of atrial fibrillation (in a paroxysm-free period), chronic IIA heart failure (functional class II), and grade 3 arterial hypertension.
The echocardiographic picture demonstrated mild mitral valve insufficiency and additional posterior mitral valve leaflet mass up to 9 mm in size located on the pedicle.
Multispiral computed tomography with bolus contrast enhancement on a Philips iCT 256-slice ECG-synchronized device and magnetic resonance imaging (MRI) of the heart on a General Electric Optima MR450w GEM 1.5 T machine were performed for a detailed mass, thoracic organs, and coronary artery assessments.
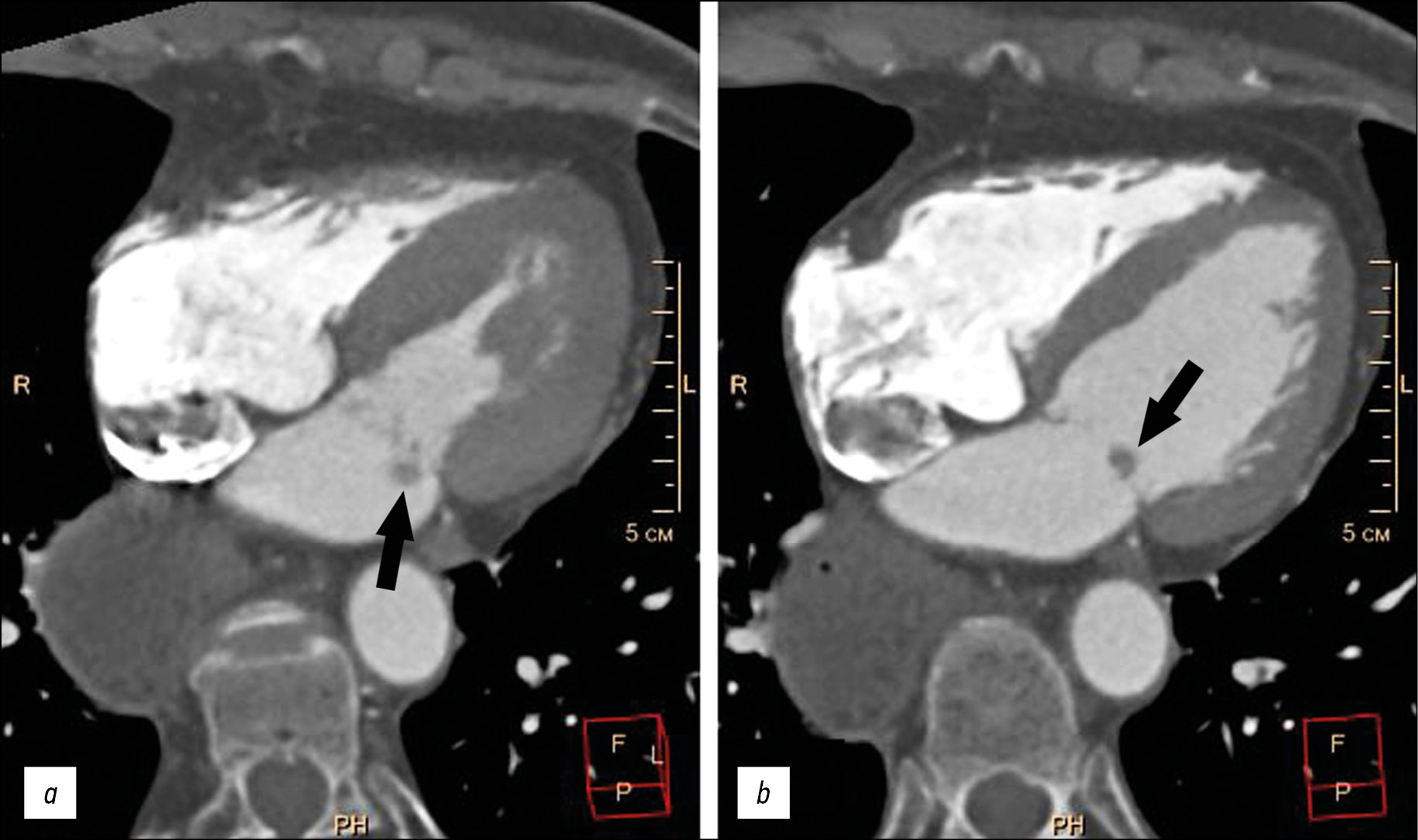
Computed tomography revealed no additional volumetric masses or areas of inflammatory infiltration in the pulmonary tissue. The stomach was visualized in the bed of the removed esophagus without pathological volumetric masses at this level. The examination revealed no pronounced coronary artery narrowings. An additional volumetric mass measuring 5–9 mm, round in shape, with clear irregular contours, and displaced together with the valve leaflet into the left ventricular cavity during atrial systole was visualized on the atrial surface of the posterior mitral valve leaflet (Fig. 1).
Fig. 1. Multispiral computed tomography of thoracic organs, four-chamber planar heart reconstruction, arterial contrast phase: а, left ventricular systolic phase; b, left ventricular diastolic phase. Additional rounded structure on the posterior mitral valve leaflet (black arrows).
A series of Fiesta-CINE functional examinations in standard axes (two- and four-chamber long axis with 8 mm slice thickness and 0 mm inter-slice interval) was performed after a series of panoramic and axial chest scans in cardiac MRI. Tumor visualization in standard cardiac MRI views was difficult because of the small size of the mass. Optimal mass visualization was obtained in the modified Fiesta-CINE two- and four-chamber views (Fig. 2).
Fig. 2. Magnetic resonance imaging of the heart, two-chamber view: a, left ventricular systolic phase; b, left ventricular diastolic phase. Additional mass on the posterior mitral valve leaflet (black arrows).
A small round-shaped mass (5 × 8 mm in size) on the posterior mitral valve leaflet on the left atrial side was confirmed. The examination was performed before and after early and delayed contrast enhancement using T2 SS, FSE, and FS pulse sequences—T2 WI with signal suppression from blood and adipose tissue—and PS MDE (PSIR), TI 250 ms postcontrast images to obtain tissue mass characteristics. A contrast agent (gadopentetic acid) was injected at 0.2 ml/ kg body weight.
After delayed contrast enhancement, an increased signal was observed compared to the native T1-WI series (Fig. 3).
Fig. 3. Magnetic resonance imaging of the heart, two-chamber view: a, native T1-WI series, TSE; b, postcontrast T1-WI series, TSE. Additional mass on the posterior mitral valve leaflet (white arrows).
The patient underwent mass excision with mitral valve suture plasty under cardiopulmonary bypass. Moreover, the postoperative period proceeded without any complications.
The histological study of the mass showed a characteristic morphological picture of a myxoma.
DISCUSSION
Myxoma is the most common primary cardiac tumor; however, the number of cases in the general population is extremely small. Moreover, myxoma, which affects the heart valve leaflets, is the rarest pathology. Such changed variants were first described in 1934 [8].
According to foreign literature, the number of described cases is precisely unknown; however, the approximate prevalence of this localization among myxomas is approximately 1.5% [9, 10].
Echocardiographic examination and MRI are the methods of choice for suspected cardiac masses. Differential diagnosis with vegetation on the heart valves and papillary fibroelastoma is necessary for an atypical tumor localization [5, 6].
The vegetations are more frequently located on the atrial surface of the mitral valve, as demonstrated in our clinical case; however, imaging techniques identified a pedicle that is more indicative of a mass. MRI with delayed contrast revealed vegetations with uneven accumulation of contrast agent, which complicated the differential diagnosis of vegetations and masses [11, 12], whereas no clinical data for infectious endocarditis with valves vegetations were available in the described case.
Papillary cardiac fibroelastoma is the second most common benign primary tumor. This mass is characterized by its small size (usually <15 mm), rounded shape, and short pedicle. Typical localization includes the atrial surface of the mitral valve or the aortic surface of the aortic valve [2, 13].
CONCLUSIONS
The reported clinical case did not reveal any specific characteristics of cardiac myxoma despite the use of modern imaging techniques. However, the presence of a mobile mass of tumorous nature required surgical treatment, after which histological examination allowed a myxoma diagnosis of an extremely rare localization.
ADDITIONAL INFORMATION
Funding source. The article had no sponsorship.
Competing interests. The authors declare that they have no competing interests.
Authors’ contribution. All authors made a substantial contribution to the conception of the work, acquisition, analysis, interpretation of data for the work, drafting and revising the work, final approval of the version to be published and agree to be accountable for all aspects of the work.
Consent for publication. Written consent was obtained from the patient for publication of relevant medical information and all of accompanying images within the manuscript.
About the authors
Marina V. Vishniakova
Moscow Regional Research and Clinical Institute
Author for correspondence.
Email: cherridra@mail.ru
ORCID iD: 0000-0003-3838-636X
SPIN-code: 1137-2991
MD, Dr. Sci. (Med)
Russian Federation, 61/2, Shepkina street, Moscow,129110Alexander S. Abramenko
Moscow Regional Research and Clinical Institute
Email: a.s.abramenko@gmail.com
ORCID iD: 0000-0002-6286-2162
SPIN-code: 9743-3001
Научный сотрудник отделения лучевой диагностики
Russian Federation, 61/2, Shepkina street, Moscow,129110Mariya V. Vishniakova
Moscow Regional Research and Clinical Institute
Email: cherridra@list.ru
ORCID iD: 0000-0002-2649-4198
SPIN-code: 7748-1831
MD, Dr. Sci. (Med)
Russian Federation, 61/2, Shepkina street, Moscow,129110Dmitry V. Shumakov
Moscow Regional Research and Clinical Institute
Email: cherridra@mail.ru
ORCID iD: 0000-0003-4204-8865
SPIN-code: 2545-2978
MD, Dr. Sci. (Med), Corresponding Member of the Russian Academy of Sciences
Russian Federation, 61/2, Shepkina street, Moscow,129110References
- Centofanti P, Di Rosa E, Deorsola L, et al. Primary cardiac tumors: early and late results of surgical treatment in 91 patients. Ann Thorac Surg. 1999;68(4):1236–1241. doi: 10.1016/s0003-4975(99)00700-6
- Hoey ET, Shahid M, Ganeshan A, et al. MRI assessment of cardiac tumours: part 1, multiparametric imaging protocols and spectrum of appearances of histologically benign lesions. Quant Imaging Med Surg. 2014;4(6):478–488. doi: 10.3978/j.issn.2223-4292.2014.11.23
- Zheltovsky YV, Batekh VI, Podkamenny VA, et al. Diagnosis and treatment with a heart mix. Acta Biomedica Sci. 2017;2(6):21–26. (In Russ).
- Lam KY, Dickens P, Chan AC. Tumors of the heart. A 20-year experience with a review of 12,485 consecutive autopsies. Arch Pathol Lab Med. 1993;117(10):1027–1031.
- Li X, Chen Y, Liu J, et al. Cardiac magnetic resonance imaging of primary cardiac tumors. Quant Imaging Med Surg. 2020;10(1):294–313. doi: 10.21037/qims.2019.11.13
- Aggeli C, Dimitroglou Y, Raftopoulos L, et al. Cardiac masses: the role of cardiovascular imaging in the differential diagnosis. Diagnostics. 2020;10(12):1088. doi: 10.3390/diagnostics10121088
- Kallstrom E, Kallus E, Erbe K, et al. Differentiation of left atrial myxomas by multimodality imaging. J Diagnostic Med Sonography. 2020;36(1):52–63. doi: 10.1177/8756479319872153
- Jaleski TC. Myxoma of the heart valves: report of a case. Am J Pathol. 1934;10(3):399–406.
- Wold LE, Lie JT. Cardiac myxomas: a clinicopathologic profile. Am J Pathol. 1980;101(1):219–240.
- Yoon JH, Kim JH, Sung YJ, et al. Cardiac myxoma originating from the anterior mitral valve leaflet. J Cardiovasc Ultrasound. 2011;19(4):228–231. doi: 10.4250/jcu.2011.19.4.228
- Rajiah P, Moore A, Saboo S, et al. Multimodality imaging of complications of cardiac valve surgeries. Radio Graphics. 2019;39(4):932–956. doi: 10.1148/rg.2019180177
- El Ouazzani J, Jandou I, Christophe Thuaire I. Thrombus or vegetation? Importance of cardiac MRI as a diagnostic tool based on case report and literature review. Ann Med Surg (Lond). 2020;60:690–694. doi: 10.1016/j.amsu.2020.12.007
- Anand S, Sydow N, Janardhanan R. Papillary fibroelastoma diagnosed through multimodality cardiac imaging: a rare tumour in an uncommon location with review of literature. BMJ Case Rep. 2017;2017:bcr2017219327. doi: 10.1136/bcr-2017-219327
Supplementary files